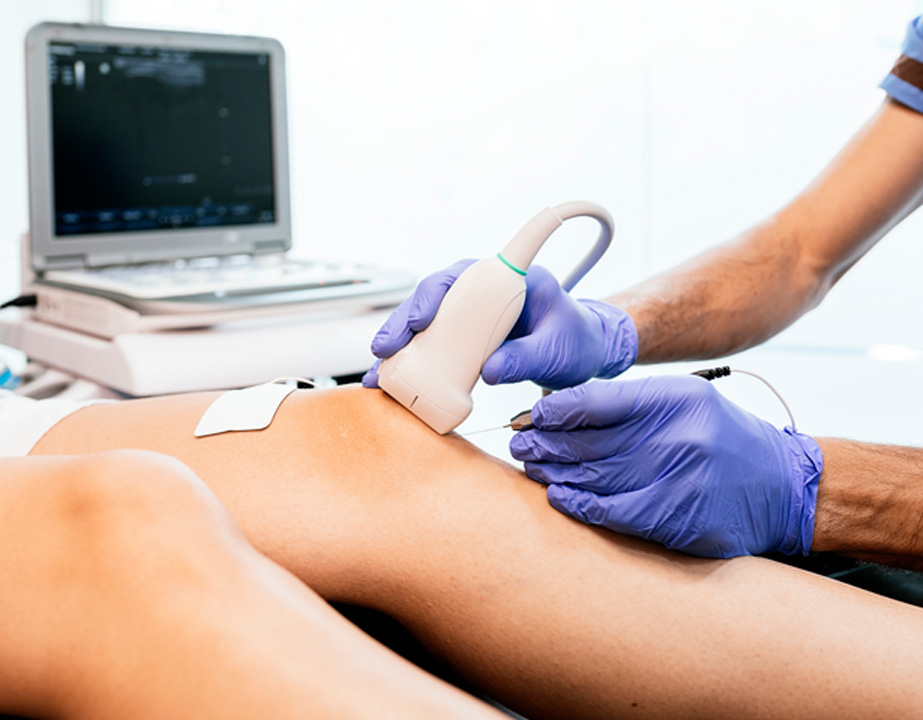
Osteoarthritis is a condition that develops when the protective cartilage that cushions the bones wears down.
The damage to the joints can’t be reversed, but symptoms can be managed.
Symptoms of Osteoarthritis
Signs of the condition include:
- Pain in the joints in the hands, knees, hips or spine
- Inability to move the joint through its full range of motion
- Joint stiffness that is most severe when waking up or moving after being inactive
- Tenderness in the joints
- Bone spurs forming around the affected joint
- Grating sensation, popping or crackling when using the joint
- Swelling
Risk Factors of Osteoarthritis
Certain individuals may be at greater risk of developing osteoarthritis if they:
- Are older
- Are female
- Are obese (increased weight adds stress to weight-bearing joints; fat tissue produces proteins that can lead to inflammation)
- Have joint injuries
- Have a genetic predisposition
- Have certain metabolic diseases
- Make repetitive motions that place repetitive stress on the joints
- Were born with malformed joints or defective cartilage
Diagnosing Osteoarthritis
Patients experiencing symptoms should schedule an appointment with their primary physician. During the initial visit, the doctor will check the affected joint for tenderness, redness, swelling, and flexibility. The doctor will recommend obtaining an X-ray and MRI of the affected joint to get a better picture of the damage.

An MRI may be useful in complex cases and provide more detailed images of bone and soft tissues.
Blood tests and joint fluid analysis may also be necessary to rule out other causes of joint pain, such as rheumatoid arthritis, gout, or an infection.
Treating Osteoarthritis
Though osteoarthritis cannot be reversed, certain treatments can improve a patient’s mobility and alleviate pain.
Medication
Patients may take acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs) to relieve pain. Stronger NSAIDs will require a prescription.
Duloxetine (Cymbalta) is an antidepressant but can also be used to treat chronic pain, including osteoarthritis pain.
Physical therapy can help patients strengthen the muscles near the affected joints, increase their flexibility and reduce pain. Patients can also engage in regular exercise on their own, such as swimming or walking.
Occupational therapy can teach patients how to perform everyday tasks without putting extra stress on their joints. The exercises will be tailored to each patient’s unique condition and needs.
Knee Intra-Articular Injections
If medication and therapy fail to provide sufficient pain relief, the patient’s physician may recommend knee intra-articular injections.
The risks of knee intra-articular injections are rare, but may include bruising, swelling, infection, skin irritation, allergic reaction to the medicine, bleeding in the joint or weakness in the leg.
What to Expect During a Knee Intra-Articular Injection Procedure
The procedure begins with the physician cleansing the injection site with an antiseptic. The physician will use ultrasonic guidance to ensure the needle is inserted in the correct place. Once the needle is correctly positioned, the local anesthetic and steroid will be injected.
Patients may receive up to three or four injections per year.

