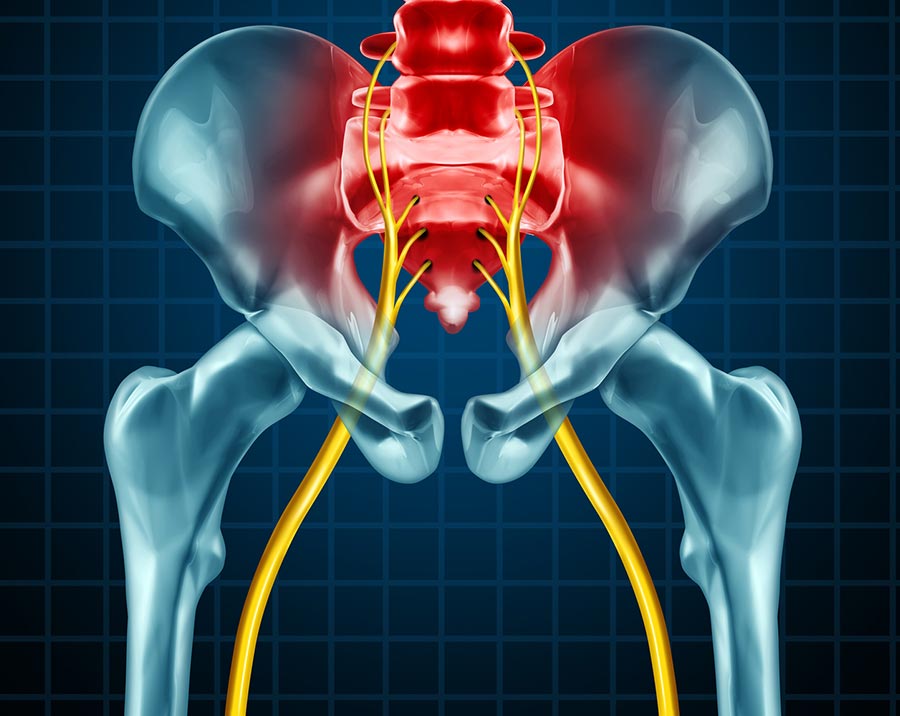
Radiculopathy is a term used to describe the symptoms produced by the pinching of a nerve root in the spinal column.
Lumbar radiculopathy occurs in the lower back and is also referred to as sciatica.
Symptoms of Radiculopathy
Symptoms of radiculopathy may include:
- Weakness or loss of reflexes in the arms or legs
- Sharp pain in the back, arms, shoulders or legs that may be exacerbated by certain activities
- Numbness of the skin, “pins and needles”, or other abnormal sensations in the arms or legs
Causes of Radiculopathy
The condition may be caused by:
- Bulging or herniated discs
- Bone spurs, or areas of extra bone growth that may be caused by inflammation from osteoarthritis, trauma or other degenerative conditions
- Thickening of the spinal ligaments
- Spinal infections
- Cancerous and noncancerous growths in the spine
Diagnosing Radiculopathy
Radiculopathy may be diagnosed by a physical exam to test muscle strength and reflexes. Pain caused by a certain movement can be used to identify the affected nerve root.
An X-ray, CT scan or an MRI scan will also be taken to help the doctor see the structures in the problem area.
Nerve conduction studies, along with electromyography, can help determine if the cause is neurological or muscular.
Benefits of a Lumbar Epidural Injection
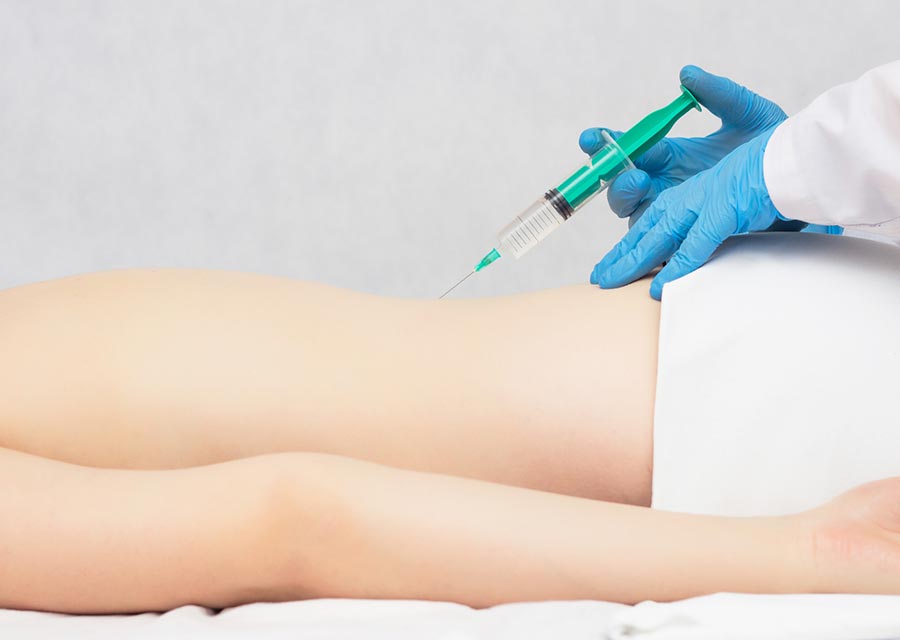
Lumbar epidural injections can be used to treat the pain caused by radiculopathy.
During the procedure, cortisone is injected into the epidural space, which is the space that surrounds the spinal sac and cushions the nerves and spinal cord. The treatment may help alleviate pain and inflammation in and around the spinal nerve roots as well as around damaged nerves.
The procedure can be performed to alleviate pain caused by:
- Post-operative “failed back” surgery syndromes
- Bone spurs
- Injuries to spinal nerves, vertebrae and surrounding tissue
- Spinal stenosis (narrowing of the spinal canal)
- Herniated or bulging discs
What to Expect During a Lumbar Epidural Injection
The procedure can be performed using one of three different methods of injecting the steroid into the epidural space: caudal, interlaminar and transforaminal. Whichever method is chosen, a thin needle will be positioned using fluoroscopic (or X-ray) guidance and contrast dye will be used to make sure the medication reaches the intended area. Local anesthetic may be added to provide temporary pain relief.
During an interlaminar injection, also known as an epidural injection, the steroid is injected into the back of the epidural space and covers a wide area.
During a caudal injection, the steroid injection is delivered to the sacral hiatus (a small opening just above the tailbone) and targets the very bottom of the epidural space. In both approaches, the steroid spreads over several spinal segments and affects both sides of the spinal canal.
During a transforaminal injection, also known as a nerve block, the steroid is injected alongside the nerve exiting the spine and the medication is delivered into the nerve sleeve. The medication reaches the epidural space through the sleeve. This method of epidural injection is useful for treating one segment or one side of the back.
Patients may feel tingling or pressure when the injection is performed. If the swelling is extensive, patients may experience a burning sensation or mild discomfort as the epidural reaches the epidural space. Once the procedure is finished, patients will rest for up to an hour and a nurse or technologist will check to make sure they are not experiencing any unfavorable reactions before leaving the facility.

