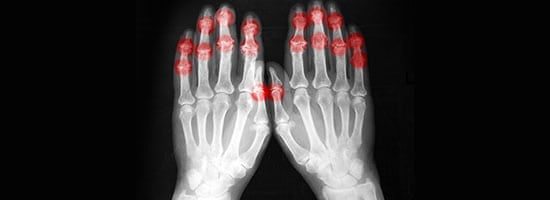
Diagnosing and Treating Osteoarthritis
Affecting more than 30 million adults, osteoarthritis (OA) is a form of arthritis that’s characterized by the gradual breakdown of the cartilage and bones of joints. Hands, hips, and knees are often affected, although it can also be a source of lower back pain if the joints of the spine (facet joints) become worn or weakened. There is no cure for osteoarthritis. However, it’s a condition that can often be effectively managed.
Who Gets Osteoarthritis?
Unlike rheumatoid arthritis, OA is not an autoimmune disease. It’s considered a chronic condition. According to the Centers for Disease Control and Prevention (CDC), most adults will have some type of OA by the time they reach their seventies. It tends to affect women more after the age of 55 due to changes within the body related to menopause such as a gradual loss of bone density. Osteoarthritis sometimes affects males under the age of 45, but this is less common.
Symptoms and Signs Suggesting Osteoarthritis
It’s the inflammation and swelling caused by the breakdown of cartilage that often makes osteoarthritis painful. As tissues wear down, there’s more friction between bones during regular movements. Usually appearing gradually as the wear and tear affects tissues, symptoms and signs that indicate OA may include:
- Noticeable loss of motion
- Stiffness or tightness around joints, especially when first waking up
- Pain associated with daily movements
- Visible swelling around joints
Diagnosis and Treatment of Osteoarthritis
Osteoarthritis is usually diagnosed based on a patient’s reported symptoms. Image tests are often performed to determine the extent of the damage to joints and supporting tissues and show where there may be excess fluid buildup.
OA is usually treated with a combination of remedies. Patients may be referred to a physical therapist for tips on how to safely exercise to strengthen muscles that support joints. Dietary changes are sometimes suggested to minimize inflammation. Treatment of OA may also involve:
- Non-steroidal anti-inflammatory drugs (NSAIDs) to reduce inflammation
- Losing excess weight to ease pressure on joints
- Short-term use of pain medications
- Use of supportive devices, such as crutches or braces, if appropriate
- Surgery in the form of joint fusion or replacement or arthroscopic procedures to remove fluid around joints or bony growths
The role of an orthopedic surgeon in the treatment of osteoarthritis is to determine the extent of the damage and determine the most effective way to manage any discomfort from it. Surgery is rarely necessary, although it may be an option if joint damage has resulted in discs slipping or joint fractures not responding to other treatments.

